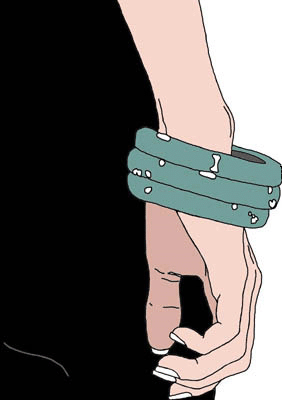
AORTIC DISSECTION
Most common in patients with a history of long-standing hypertension, cocaine use, or aortic root disease such as Marfan's syndrome or Takayasu's arteritis.
Symptoms
- Sudden-onset severe chest pain, sometimes radiating to the back.
- May present with neurologic symptoms from occlusion of vessels supplying the brain or spinal cord.
Exam
Look for any of the following: aortic regurgitation, asymmetric pulses, neurologic findings.
Differential
MI, pulmonary embolus, pneumothorax.
Diagnosis
Requires a high index of suspicion. CXR has low sensitivity but may show a widened mediastinum or a hazy aortic knob. CT scan with IV contrast is diagnostic and shows the extent of dissection. Transesophageal echocardiography (TEE) is highly sensitive and specific.
Always think about dissection in patients with chest pain!
Treatment
-
Initial medical stabilization: Aggressive HR and BP control with β-blockers first (typically IV propranolol), followed by IV nitroprusside if needed.
- Ascending dissection (type A): Emergency surgical repair.
-
Descending dissection (distal to the left subclavian artery — type B): Medical management unless there is intractable pain, progressive dissection, or vascular occlusion of aortic branches.
Complications
Aortic rupture, acute aortic regurgitation, tamponade, neurologic impairment, limb or mesenteric ischemia, renal ischemia.
HYPERCHOLESTEROLEMIA
One of the major contributors to atherosclerotic vascular disease. An ↑ LDL and a low concentration of HDL are the 1° contributors.
Symptoms
Asymptomatic unless the patient develops ischemia (e. g., angina, stroke, claudication) or unless severe hypertriglyceridemia → pancreatitis.
Exam
-
Look for evidence of atherosclerosis — e. g., carotid, subclavian, and other bruits; diminished pulses; ischemic foot ulcers.
- Look for xanthomas (lipid depositions) over the tendons, above the upper eyelid, and on the palms.
Differential
Hypercholesterolemia can be idiopathic, genetic or 2° to other diseases, such as diabetes, nephrotic syndrome, and hypothyroidism.
Diagnosis
- Based on a lipid panel. A full fasting lipid panel consists of total cholesterol, HDL, LDL, and triglycerides.
-
Because triglycerides rise following a meal, only total cholesterol and HDL can be measured after a meal. Triglycerides and LDL can be measured only when fasting.
-
LDL is not measured directly; it is calculated on the basis of total cholesterol, HDL, and triglycerides. High triglycerides (> 400) make LDL calculation unreliable.
-
Look for other contributing conditions. Check glucose and TSH; check body weight; consider nephrotic syndrome.
Treatment
Treatment is aimed at preventing pancreatitis when triglycerides are very high as well as at preventing atherosclerotic disease (see Table 2.2-1).
Table 2.2-1. Mechanisms and Side Effects of Cholesterol-Lowering Medications.
Medication | Primary Effect | Side Effect | Comments |
| HMG-CoA reductase inhibitors ("statins") | ↓ LDL | Hepatits, myositis. | Potent LDL-lowering medication. |
| Cholesterol absorption inhibitors (ezetimibe) | ↓ LDL | Introduced in 2003; its role in therapy is being defined. | |
| Fibrates (gemfibrozil) | ↓triglycerides, slightly ↑ HDL | Potentiates myositis with statins. | |
| Bile acid-binding resins | ↓ LDL | Bloating and cramping. | Most patients cannot tolerate GI side effects. |
| Nicotinic acid (niacin) | ↓ LDL, ↑ HDL | Hepatitis, flushing. | Aspirin before dose ↓ flushing. |
-
Triglycerides: If > 500, recommend dietary modification (↓ total fat and ↓ saturated fat) and aerobic exercise, and begin medication (fibrate or nicotinic acid). At lower levels, treatment can begin with diet and exercise, and medication can be added as needed. Treat diabetes if present.
-
LDL: In patients with diabetes or CAD, the goal LDL is < 100. The mainstay of treatment is diet, exercise, and a statin. LDL control is the 1° cholesterol-related goal in patients with CAD or diabetes.
-
HDL: Can be modestly ↑ with fibrate or nicotinic acid.
CORONARY ARTERY DISEASE (CAD)
Atherosclerotic occlusion of the coronary arteries. Major risk factors are age, family history, smoking, diabetes, hypertension, and high cholesterol.
Symptoms
- Asymptomatic.
-
Stable angina: Chest tightness/pain or shortness of breath with a consistent amount of exertion; relief with rest or nitroglycerin. Reflects a stable, flow-limiting plaque.
-
Unstable angina (acute coronary syndrome): Chest tightness/pain and/or shortness of breath, typically at rest, that does not improve with nitroglycerin. Reflects a plaque that has ruptured with formation of a clot in the lumen of the blood vessel.
Exam
- Exam can be normal when the patient is asymptomatic.
- Look for signs of heart failure (↑JVD, bibasilar crackles, lower extremity edema) from prior MI.
-
Look for vascular disease elsewhere — e. g., bruits, asymmetric pulses, and lower extremity ischemic ulcers.
Differential
See the diffferential for MI below.
Diagnosis
-
Stress testing: Exercise or dobutamine to ↑ HR: ECG, echocardiogram, or radionuclide to assess perfusion (see the section on stress testing below).
- Cardiac catheterization: Defines the location and severity of lesions.
Treatment
- To slow progression: Control diabetes, ↓ BP, ↓ cholesterol (goal low-density cholesterol < 100), stop smoking.
- To prevent angina: β-blockers ↓ BP and ↓ cardiac workload, which will ↓ exertional angina. If symptoms arise on a β-blocker, a long-acting nitrate or calcium channel blocker can be added.
- To prevent MI: Aspirin; clopidogrel for aspirin-sensitive patients.
ENDOCARDITIS
Inflammation of the heart valves; can be infectious or noninfectious. Infectious endocarditis is commonly seen in IV drug abusers and in those with valvular lesions or prosthetic heart valves.
Symptoms
-
Acute endocarditis: Fever, rigors, heart failure from valve destruction, symptoms related to systemic emboli (neurologic impairment, back pain, pulmonary symptoms).
-
Subacute bacterial endocarditis: Weeks to months of fever, malaise, and weight loss. Also presents with symptoms of systemic emboli.
- Noninfectious endocarditis: Generally asymptomatic. Can cause heart failure by destroying valves.
Exam
New murmur. Findings associated with emboli include focal neurologic deficits and tenderness to percussion over the spine. With infectious endocarditis, look at the fingers and toes for deep-seated, painful nodules (Osler's nodes = "Ouch"ler's nodes) and small skin infarctions (Janeway lesions). Retinal exudates are called Roth's spots.
Differential
The differential diagnosis of endocarditis is outlined below and in Table 2.2-2.
Table 2.2-2. Causes of Endocarditis.
Acute | Subacute | Culture Negative | NBTE (marantic endocarditis) | Verrucous Endocarditis (Libman-Sacks) |
| Most commonly S. aureus. | Viridans streptococci, Enterococcus, S. epidermidis, gram-negative rods, Candida. | HACEK organismsa, Coxiella burnetii, noncandidal fungi. | Thrombus formation on valve seen in many cancers. | Seen in lupus; vegetation composed of fibrin, platelets, immune complexes, and inflammatory cells. |
aHACEK = Haemophilus aprophilus and H. parainfluenzae, Actinobacillus actinomycetemcomitans, Cardiobacterium hominis, Eikenella corrodens, Kingella kingae.
-
Differential of a vegetation found on echocardiography: Infectious endocarditis, nonbacterial thrombotic endocarditis (NBTE, or marantic endocarditis), verrucous endocarditis (or Libman-Sacks endocarditis), valve degeneration.
-
Differential of bacteremia: Infectious endocarditis, infected hardware (e. g., from a central line), abscess, osteomyelitis.
Diagnosis
-
The discovery of noninfectious endocarditis is usually an incidental finding on echocardiography. It may be found during the workup of systemic emboli.
-
Infectious endocarditis is diagnosed by a combination of lab and clinical data. If suspicious, obtain three sets of blood cultures and an echocardiogram. If the transthoracic echocardiogram is (-), proceed to TEE (more sensitive). (+) blood cultures and echocardiogram findings diagnose endocarditis.
Any patient with S. aureus bacteremia should be evaluated for endocarditis with echocardiography.
Treatment
-
Prolonged antibiotics, generally for 4-6 weeks. Begin empiric therapy with gentamicin and antistaphylococcal penicillin (oxacillin or nafcillin). If there is a risk of methicillin-resistant S. aureus, use vancomycin instead of oxacillin/nafcillin.
-
Valve replacement for fungal endocarditis, heart failure from valve destruction, valve ring abscess, or systemic emboli despite adequate antibiotic therapy.
- Following treatment for infectious endocarditis, patients should receive endocarditis prophylaxis.
- NBTE: Treat the underlying disorder. Heparin is useful in the short term.
- Verrucous: No treatment is required. Patients should receive endocarditis prophylaxis (see below).
Complications
Spinal osteomyelitis, valve destruction and heart failure, embolic stroke.
Prevention
Give endocarditis, prophylaxis to patients who are undergoing procedures associated with a risk of bacteremia (see Tabe 2.2-3) and have any of the following risk factors:
- Prosthetic valves (mechanical or bioprosthetic).
- Prior bacterial endocarditis.
- Acquired valve dysfunction.
- Most congenital heart abnormalities.
- Hypertrophic cardiomyopathy.
- Mitral valve prolapse with mitral regurgitation.
Table 2.2-3. Selected Procedures Carrying a Risk of Bacteremia.
Dental:
Pulmonary:
GI:
GU:
|
Prophylaxis regimens are as follows:
- Amoxicillin (clindamycin if penicillin allergy) one hour before the procedure.
- If the patient is undergoing a GI or GU and has a high-risk valve lesion (e. g., a prosthetic valve, prior endocarditis, or congenital heart abnormalities that cause cyanosis), cover Enterococcus with IV ampicillin and gentamicin.
HEART FAILURE (CONGESTIVE HEART FAILURE)
Inability of the heart to pump adequate blood to meet the needs of the body. Can be categorized in different ways. One such categorization is as follows:
- Systolic dysfunction.
- Diastolic dysfunction.
- Valvular dysfunction.
- Arrhythmia causing heart failure.
Systolic Heart Failure
Weakened pumping function of the heart muscle. Common causes include ischemic heart disease, long-standing hypertension, and viral or idiopathic cardiomyopathy in younger patients.
Symptoms
- Poor exercise tolerance, dyspnea on exertion, easy fatigability.
-
If patients are volume overloaded, they may present with orthopnea, paroxysmal nocturnal dyspnea, and ankle swelling.
Exam
- Bibasilar crackles.
- Diffuse PMI that is displaced to the left (reflects cardiomegaly).
- S3 gallop.
- ↑ JVD (normal is about 0-2 cm vertical elevation above the sternomanubrial junction).
- Lower extremity edema.
Differential
- Deconditioning.
- Lung disease (e. g., COPD).
- Heart failure of other types (e. g., diastolic dysfunction).
- Other causes of edema (e. g., low albumin and nephrotic syndrome).
Diagnosis
History and exam are suggestive, but determination of the ejection fraction via an imaging study is the definitive diagnosis:
- Echocardiogram.
- Radionuclide imaging (e. g., thallium).
-
Look for the cause of the low ejection fraction: Perform a stress test or cardiac catheterization to look for CAD; test for TSH levels and for HIV. Look for a history of alcohol use or exposure to offending medications such as doxorubicin; may perform myocardial biopsy.
Ventricular tachycardia is a common cause of death in patients with a ↓ ejection fraction.
Treatment
- Maintenance medications:
- β-blockers: Metoprolol, atenolol, others.
- Afterload reduction: Ideally an ACEI or an angiotensin receptor blocker (ARB).
- Spironolactone if the patient's potassium can tolerate it.
- Digoxin is falling out of favor because it has toxicities and does not improve morality.
- Exacerbations: Loop diuretics such as furosemide when the patient is volume overloaded.
- Other:
-
Automatic implantable cardiac defibrillator (AICD): Associated with ↓ mortality from ventricular tachycardia, but very expensive.
- Treat the cause of the systolic heart failure, such as CAD.
ACEIs, ARBs, and spironolactone all cause hyperkalemia.
Diastolic Heart Failure
During diastole, the heart is stiff (↓ compliance) and does not relax well, resulting in ↑ diastolic filling pressure. Hypertension with ventricular hypertrophy is the most common cause; uncommon causes include infiltrative diseases such as amyloidosis and sarcoidosis.
Symptoms
The same as those for systolic heart failure.
Exam
Similar to that for systolic failure. Listen for an S4 rather than an S3.
Differential
The same as that for systolic heart failure.
Diagnosis
Presents with symptoms of heart failure with a normal ejection fraction on echocardiogram. Echo usually shows ventricular hypertrophy.
Treatment
- Control hypertension.
-
Give diuretics to control volume overload, but avoid overdiuresis, which ↓ preload and therefore cardiac output.
Active ischemia can acutely worsen diastolic dysfunction, so treat any coexisting CAD!
Valvular Causes of Heart Failure
- Right-sided valvular lesions do not typically cause heart failure.
-
In left-sided valvular lesions, aortic stenosis or aortic regurgitation and mitral stenosis or mitral regurgitation can each cause symptoms of heart failure.
- See the section on valvular disease for more detail.
Arrythmia Causing Heart Failure
This cause of heart failure is generally apparent from palpitations or ECG. Rhythms that can cause symptoms of heart failure include atrial fibrillation and bradyarrhytmias. Others present abruptly with palpitations, shortness of breath, or even syncope.
HYPERTENSION
One of the major contributors to cardiovascular disease; more common with increasing age and in blacks.
Symptoms
Asymptomatic unless severe. If severe, patients may complain of chest tightness, shortness of breath, headache, or visual disturbances.
Exam
BP > 140/90. A displaced PMI or an S4 indicates LVH. Fundi show AV nicking and "copper-wire" changes to the arterioles. Listen for bruits, which indicate peripheral vascular disease. In severe hypertension, look for papilledema and retinal hemorrhages.
Differential
Most cases are essential hypertension, but consider causes of 2° hypertension:
-
Endocrine causes: Cushing's syndrome, Conn's syndrome (aldosterone-producing tumor), hyperthyroidism.
- Chronic renal failure.
- Renal artery stenosis (listen for abdominal bruit).
- Young patients: Fibromuscular dysplasia of the renal arteries, aortic coarctation.
- Medications: OCPs, NSAIDs.
Diagnosis
BP > 140/90 on two separate occasions (elevation of either systolic or diastolic BP). A systolic BP of 120-139 or a diastolic BP of 80-89 is considered "prehypertension" and predicts the development of hypertension.
Treatment
- Goal: BP < 140/90. In diabetics and those with renal insufficiency, the goal is < 130/80.
- Interventions:
- Step 1 — lifestyle modification: Weight loss, exercise, ↓ sodium intake.
- Step 2 — medications: Begin with a thiazide unless there is an indication for another class (see Table 2.2-4).
- Control other cardiovascular risk factors, such as diabetes, smoking, and high cholesterol.
Table 2.2-4. Antihypertensive Medications.
Commonly Used Classes | Optimal Use | Main Side Effects |
| Thiazide diuretics | First-line treatment if no indication for other agents. | ↓ excretion of calcium and uric acid. |
| β-blockers | Low ejection fraction, angina. | Bradycardia, erectile dysfunction, bronchospasm in asthmatics. |
| ACEIs | Low ejection fraction, chronic kidney disease, diabetes with microalbuminuria. | Cough, angioedema, hyperkalemia. |
| ARBs | Same as ACEIs; cough with ACEI. | Hyperkalemia. |
| Calcium channel blockers | Second-line agent. | Lower extremity edema. |
Complications
Long-standing hypertension contributes to renal failure, heart failure (systolic and diastolic), CAD, peripheral vascular disease, and stroke.
MYOCARDIAL INFARCTION (MI)
Sudden rupture of an atherosclerotic plaque with partial or complete occlusion of the coronary artery. Less commonly from coronary vasospasm seen with cocaine.
Symptoms
The classic symptom of crushing substernal chest pressure radiating to the jaw or left shoulder applies mainly to middle-aged men; older men, women, and diabetics often present with nonspecific symptoms such as dyspnea, nausea, and diaphoresis.
Diabetics, women, and older men often present with dyspnea, diaphoresis, and nausea rather than with chest pain.
Exam
- Diaphoresis.
-
Bibasilar crackles or a new S3 indicates a low ejection fraction. Low blood pressure suggests cardiogenic shock.
Differential
- Always think of pneumothorax, pulmonary embolus, and aortic dissection.
-
Others: Esophageal spasm, peptic ulcer, cholecystitis, bronchospasm, pneumonia, costochondritis, pericarditis.
Diagnosis
-
Look for other causes of chest pain — take a history! Check CXR, check BP in both arms, and ask about pain radiation to the back.
-
ECG: Look for > 1-mm ST-segment elevation in contiguous leads (see Figure 2.2-1) or a new left bundle branch block.
-
Serial cardiac enzymes: Evaluate CK, CK-MB, and troponin. All begin to rise within a few hours. Troponin is nearly 100% specific for myocardial injury (also expect it to be (+) with myocarditis, cardiac contusion, etc.).
-
(+) cardiac enzymes with a nondiagnostic ECG: Called "non-ST-elevation MI", or NSTEMI. Indicates that the ruptured plaque did not completely occlude the coronary lumen but that myocardium is dying nonetheless.
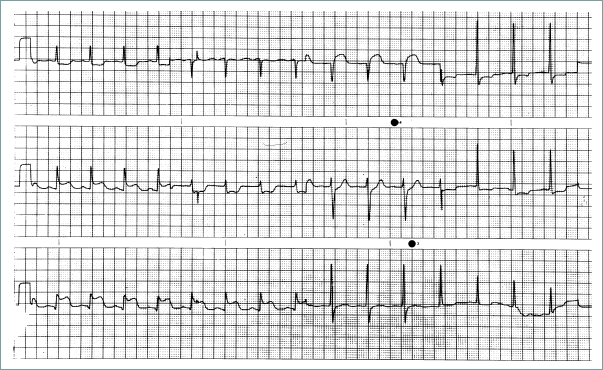
Figure 2.2-1. Myocardial infarction.
Low blood pressure with bradycardia and clear lungs indicates right ventricular infarction with sinus node ischemia.
Treatment
- ST-elevation MI (STEMI):
-
Immediately: Aspirin, IV β-blocker (↓ HR to 60 if BP will tolerate), O2, heparin. If the patient is still in pain, give IV morphine or nitrates.
-
As soon as possible: Revascularize. Cardiac catheterization with angioplasty when available, or thrombolytics if angioplasy is not available.
-
Within the first day: Begin oral β-blockers, ACEIs (if BP tolerates). The role of empiric statin use is unclear, but it is probably beneficial.
-
Long term: Treat CAD with aspirin, β-blockers, and statins (if LDL > 100). If ejection fraction is low, treat systolic dysfunction with an ACEI or ARB and spironolactone.
- NSTEMI — a bit more complicated:
-
Immediately: As above for immediate treatment of STEMI, except that low-molecular-weight heparing (enoxaparin) is preferred over unfractionated heparin.
-
Glycoprotein IIb/IIIa inhibitors (e. g., eptifibatide of abciximab) should be given to all patients who will undergo catheterization or who are at high risk as suggested by ongoing pain, stuttering chest pain, or ST depression with pain.
-
As soon as possible: Revascularize with angioplasty. If this is not possible, do not give thrombolytics! If the patient will not go to bypass surgery, give clopidogrel!
- Long term: As above.
Absolute contraindications to thrombolytics:
- Internal bleeding.
- An ischemic stroke within the past year.
- A hemorrhagic stroke at any time.
- Aortic dissection.
- Intracranial neoplasm.
Complications
-
If a patient suddenly becomes short of breath, think of papillary muscle rupture → sudden mitral regurgitation, ventricular wall rupture → left-to-right shunt (ruptured ventricular septum), or cardiac tamponade (free wall rupture).
- If chest pain recurs, think about reocclusion or pericarditis.
- Ventricular arrhythmias are a serious risk in the post-MI period.
PERICARDITIS
Inflammation of the pericardial sac. The many causes include viral infection, mediastinal radiation, MI, cancer, rheumatologic diseases (SLE), and idiopathic pericarditis.
Symptoms
Positional chest pain that is often improved by sitting up. If a large effusion is present, the patient may be short of breath.
Exam
Exam may reveal a pericardial friction rub.
Differential
Myocardial ischemia, aortic dissection, pneumonia, pulmonary embolism, pneumothorax.
Diagnosis
- Diffuse ST-segment elevation on ECG (see Figure 2.2-2).
- Echocardiogram may reveal an associated effusion.
-
Search for an underlying cause — take a history for viral ilness, radiation exposure, and malignancy. Check antinuclear antibodies, PPD, blood cultures if febrile, and renal function.
Finding ST-segment elevation in numerous ECG leads will help distinguish pericarditis from MI.
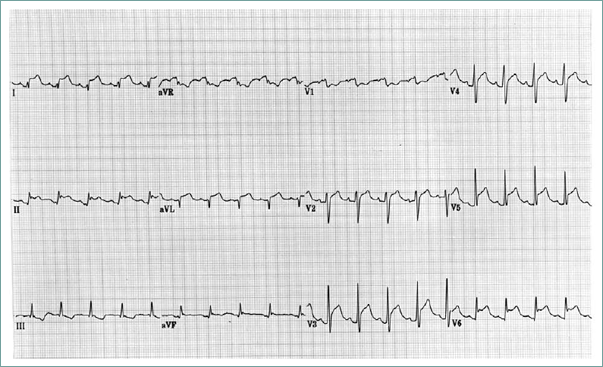
Figure 2.2-2. Pericarditis.
Treatment
- When possible, treat the underlying disorder, such as SLE or advanced renal failure.
-
For viral or idiopathic pericarditis, give NSAIDs or aspirin. Avoid NSAIDs in post-MI pericarditis because they may interfere with scar formation.
Complications
Patients can develop a clinically significant pericardial effusion and tamponade.
PERIPHERAL VASCULAR DISEASE
Atherosclerotic disease of vessels other than the coronary arteries. Risk factors are similar to those for CAD: smoking, diabetes, hypercholesterolemia, hypertension, and increasing age.
Symptoms
Depends on the organ affected.
- Mesenteric ischemia: Postprandial abdominal pain and food avoidance.
- Lower extremity: Claudication, ulceration.
- Kidneys: Usually asymptomatic, but may present with difficult-to-control hypertension.
- CNS: Stroke and TIA (see the Neurology chapter).
Exam
-
Mesenteric disease: No specific findings. The patient may be thin because of weight loss from avoiding food.
-
Lower extremity disease: Ulcers, diminished pulses, skin atrophy and loss of hair, and bruits over affected vessels (abdominal, femoral, popliteal).
- Renal artery stenosis: Listen for bruit during systole and diastole (highly specific).
Differential
-
Abdominal pain: Stable symptoms can mimic PUD or biliary colic. If the colon is predominantly involved, episodes of pain and bloody stool can look like infectious colitis.
-
Lower extremities: Spinal stenosis can produce lower extremity discomfort similar to claudication. Claudication improves with standing still, but spinal stenosis classically improves with sitting (lumbar flexion improves spinal stenosis symptoms).
Diagnosis
- Mesenteric disease: A diagnosis of exclusion. Angiography reveals lesions.
-
Lower extremity disease: Ankle-brachial index (compares BP in the lower and upper extremity), Doppler ultrasound. Angiography or MRA is used in preparation for revascularization but is generally not used for diagnosis.
- Renal artery stenosis: Angiography, MRA, or ultrasound with Doppler flow (technically difficult).
Acute vessel occlusion from an embolus or an in situ thrombus presents with sudden pain (abdominal or extremity) and is an emergency.
Treatment
- Control risk factors, especially smoking.
- Mesenteric disease: Surgical revascularization or angioplasty.
-
Lower extremity disease: Exercise to improve functional capacity, surgical revascularization, and sometimes angioplasty. Cilostazol is moderately useful (improves pain-free walking distance 50%); while pentoxifylline has marginal benefit.
- Renal artery stenosis: Surgery or angioplasty might be useful.
STRESS TESTING
Indications for stress testing are as follows (not a comprehensive list):
- Diagnosis of CAD/evaluation of symptoms.
- Preoperative evaluation.
- Risk assessment in patients with known disease.
- Decision making about the need for revascularization.
Contraindications (not a comprehensive list) include the following:
- Severe aortic stenosis.
- Unstable coronary syndrome.
- Decompensated heart failure.
Testing consists of a stressing modality and an evaluating modality (see Tables 2.2-5 and 2.2-6).
Table 2.2-5. Stressing Modalities in Cardiac Testing.
Stressing Modality | Pros | Cons |
| Treadmill | Good for patients who can walk. | |
| Dobutamine | Good for patients who cannot exercise. | |
| Adenosine or dipyridamole (with nuclear imaging) | Good for patients who cannot exercise. | Can cause bronchospasm — be cautious in patients with COPD. |
Table 2.2-6. Evaluating Modalities in Cardiac Testing.
Evaluating Modality | Pros | Cons |
| ECG | Inexpensive. | Cannot localize the lesion; cannot use with baseline ST-segment abnormalities or left bundle branch block. |
| Echocardiogram | Good in patients with left bundle branch block; cheaper than nuclear imaging | Technically limited echo images or resting wall motion abnormalities can limit usefulness. |
| Radionuclide tracer (thallium or technetium) | Localizes ischemia; localizes infarcted tissue. | Expensive. |
- The stressor can be walking on a treadmil or IV dobutamine.
- Evaluating modalities are ECG, echocardiogram, and nuclear imaging such as thallium.
-
An additional testing method is adenosine or dipyridamole with nuclear imaging. Adenosine and dipyridamole dilate the coronary arteries, but areas with plaque cannot vasodilate. These agents thus ↑ blood flow in healthy arteries but cause no change in diseased arteries, creating a differential flow that is detected on nuclear imaging.
CARDIAC TAMPONADE
Small-volume fluid collections can cause symptoms if they accumulate quickly. Gradually developing collections can accumulate 1-2 L before causing symptoms. Common causes include pericarditis with effusion, ventricular free wall ruprure, aortic dissection extending to the aortic root, and trauma.
Symptoms
- Shortness of breath, syncope.
- Symptoms associated with the underlying process, such as chest pain with an MI.
Think of tamponade in any patient with pulseless electrical activity.
Exam
↑ JVP is found in nearly 100% of patients. Also presents with hypotension, tachycardia, pulsus paradoxus (a drop in systolic BP during inspiration > 10 mmHg), and muffled heart sounds.
Differential
- Acute development: Pulmonary embolus, MI, tension pneumothorax.
- Gradual development: Heart failure, lung disease.
Diagnosis
CXR may show a large cardiac silhouette if there is a large-volume effusion; ECG may show low voltage. Echocardiogram shows effusion and may show right atrial or right ventricular dynamic collapse in diastole.
Treatment
If there is a hemodynamic compromise, treat with IV fluids and urgent pericardiocentesis. For recurrent effusions, a pericardial window may be needed.
VALVULAR DISEASE
All valve lesions need endocarditis prophylaxis except mitral valve prolapse.
Table 2.2-7 describes the clinical characteristics and treatment of common valvular lesions.
Table 2.2-7. Presentation and Treatment of Select Valvular Lesions.
Lesion | Symptoms | Exam | Treatment | Comments |
| Mitral stenosis | Symptoms of heart failure, hemoptysis. | Diastolic murmur, opening snap. | HR control, balloon valvuloplasty, valve replacement. | Usually caused by rheumatic fever. |
| Mitral regurgitation | Usually asymptomatic unless severe or acute; then symptoms of heart failure. | Blowing systolic murmur at the apex, radiating to the axilla. | If acute, usually needs surgery. For chronic mitral regurgitation, repair or replace the valve when symptomatic or if the ejection fraction is falling. | Long-standing regurgitation dilates the atrium, ↑ the chance of atrial fibrillation. |
| Mitral valve prolapse | Asymptomatic. | Midsystolic click; also murmur if mitral regurgitation is present. | Endocarditis prophylaxis only with mitral regurgitation. | Questionable association with palpitations and panic attacks. |
| Aortic stenosis | Chest pain, syncope, heart failure. | Harsh systolic murmur radiating to the carotids. Small and slow carotid upstroke (parvus et tardus) with severe stenosis. | Avoid overdiuresis; avoid vasodilators such as nitrates and ACEIs. Surgery for all symptomatic patients. | Once symptoms appear, mortality is 50% at three years. |
| Aortic regurgitation | Usually asymptomatic until advanced; then symptoms of heart failure. | Wide pulse pressure. Soft, high-pitched diastolic murmur. | Afterload reduction with ACEIs, hydralazine. Valve replacement if symptomatic or ↓ ejection fraction. | Many cases are associated with aortic root disease, dissection, syphilis, ankylosing spondylitis, and Marfan's. |
